Total Therapy Blog
Why You Should Put Down the Aspirin – and Build a Better Back Instead

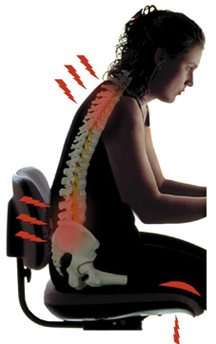
It’s a statistic that’s frequently quoted: 80% of Canadians experience low back pain. The causes of our collective back pain are diverse – poor posture, general deconditioning, weak core muscles, injury, and disease are all potential culprits. However, we exhibit a startling collective response to back pain: we take painkillers to deal with it.
A study published in the Spine Journal showed that of 219 people who saw their general practitioner for low back pain, 69% received a prescription for non-steroidal anti-inflammatory drugs (NSAIDS – e.g. aspirin, ibuprofen, naproxen), 12% received narcotics, and 4% received a prescription for acetaminophen. Only 20% did not receive a prescription for medication (Journal – Spine LWW).
 That’s not to say that pain medication isn’t an appropriate – and sometimes necessary – way to cope with back pain. But that’s the problem – it’s just a coping mechanism. Pain medication does not address the cause of back pain. Moreover, prolonged pain medication use is linked to serious health risks. NSAID use in the United States causes 16,500 deaths and 103,000 hospitalizations, annually. In fact, NSAID use is linked to more deaths annually than AIDS or cervical cancer – something most of us don’t think about when we’re reaching for the aspirin bottle. (American Gastroenterological Association)
That’s not to say that pain medication isn’t an appropriate – and sometimes necessary – way to cope with back pain. But that’s the problem – it’s just a coping mechanism. Pain medication does not address the cause of back pain. Moreover, prolonged pain medication use is linked to serious health risks. NSAID use in the United States causes 16,500 deaths and 103,000 hospitalizations, annually. In fact, NSAID use is linked to more deaths annually than AIDS or cervical cancer – something most of us don’t think about when we’re reaching for the aspirin bottle. (American Gastroenterological Association)
So what are the millions of Canadians with back pain to do? The first step to addressing back pain is to understand its cause. Was it a traumatic injury, or a repetitive strain issue? Is there an underlying illness or degenerative disorder contributing to the problem? Do you have a previous history of back pain, and if so, what was done to address it?
In order to answer these questions, you should seek out a healthcare practitioner with experience in treating patients with back pain. This can include your chiropractor, family doctor, or physiotherapist. Your healthcare practitioner will assess you to determine what the cause is, and whether or not any further imaging or intervention is required.
 Treatment plans vary depending on the issue and the individual. As a general rule, the earlier an intervention can be started, the shorter the recovery period. Treatment for low back pain can include targeted strengthening exercises to address spinal instability and reduce the wear-and-tear on the spine and pelvis. Other types of treatment may involve manual therapy to release shortened or spasming muscles, to mobilize locked joints, or to realign skeletal segments. Less frequently, more invasive treatment involving injections or surgery may be required. Surgery is generally a last resort for most mechanical sources of back pain, because it involves considerable risk on the part of the patient and produces mixed results with respect to the resolution of back pain (Journal – Spine LWW).
Treatment plans vary depending on the issue and the individual. As a general rule, the earlier an intervention can be started, the shorter the recovery period. Treatment for low back pain can include targeted strengthening exercises to address spinal instability and reduce the wear-and-tear on the spine and pelvis. Other types of treatment may involve manual therapy to release shortened or spasming muscles, to mobilize locked joints, or to realign skeletal segments. Less frequently, more invasive treatment involving injections or surgery may be required. Surgery is generally a last resort for most mechanical sources of back pain, because it involves considerable risk on the part of the patient and produces mixed results with respect to the resolution of back pain (Journal – Spine LWW).
Your treating therapist will go over your diagnosis and treatment options with you. It’s extremely important that you take an active part in your treatment. In most cases, successful treatment of low back pain requires lifestyle modifications to facilitate healing. Think of it this way – you may spend only an hour a week at therapy. What you do for the other 167 hours in your week will have a big impact on your progress. If you’re engaging in harmful or counterproductive behaviour outside of your therapy appointments, no treatment plan – no matter how sound or well-planned – will give you the results you want. Conversely, if you work closely with your therapist and actively follow their recommendations, your back pain will resolve faster than if you take a more passive role.
The bottom line is, the cause of back pain is as diverse and as individual as the person suffering with it. There is no one-size-fits-all solution, so why should we rely on a one-pill-fits-all approach?







Follow Us!
& Stay Up To Date
BLOG